There’s no doubt that overdose deaths are on the rise across the United States. This highlights the need for increased resources and interventions to address this devastating issue. According to the CDC (1), there were 70,237 overdoses in the US in 2017 – a staggering figure that demonstrates the severity of this crisis. The rise in overdoses has created the impetus for states to search for solutions to tackle this public health emergency. State initiatives to reduce overdose deaths in California are occurring, as well as in many other states. These initiatives are part of efforts to reverse this troubling trend.
The Current Opioid Crisis in California
To understand why initiatives to reduce overdose deaths in California are crucial, let’s take a look at how serious the issue has become for our country and in California.
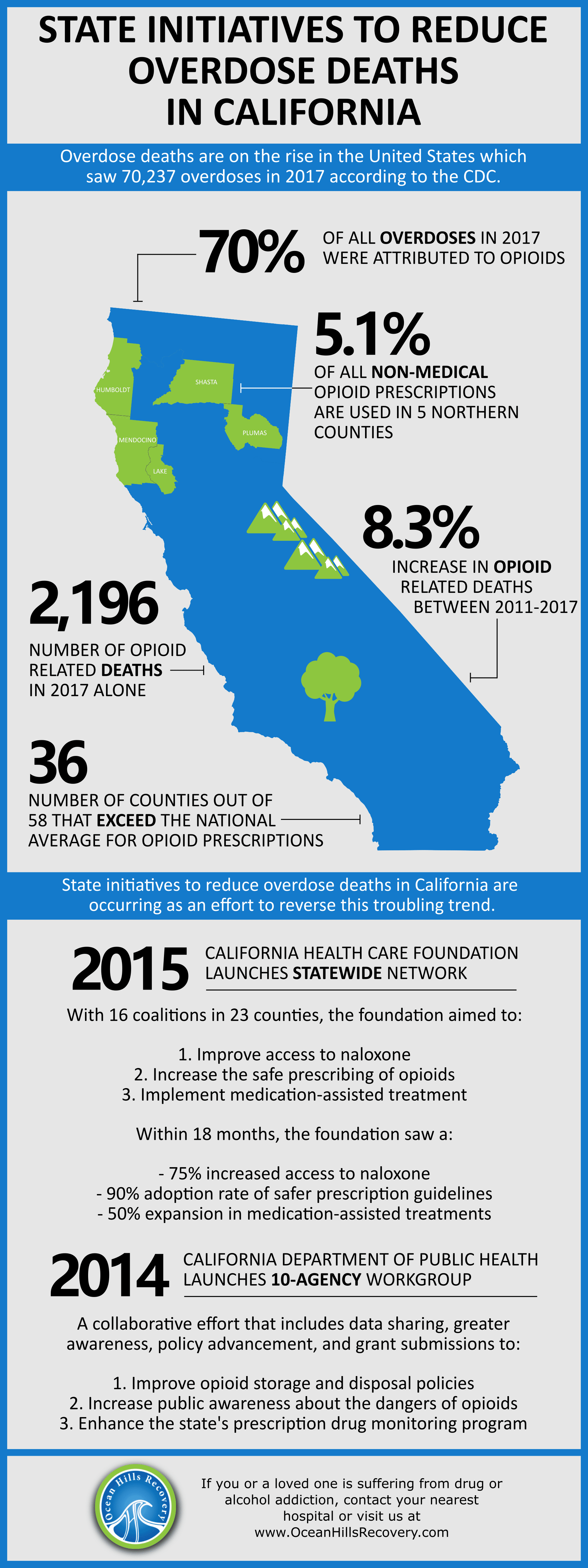
Of the 58 counties in the state, 36 exceeded the national average for the number of opioid prescriptions given to residents (2). Rural Northern California is where opioid prescriptions are their highest. 5.71% of residents in a five-county region of Humboldt, Lake, Mendocino, Plumas, and Shasta reported non-medical use of prescription drugs in the past year. These same counties also had the highest incidence of overdose deaths from prescription opioids in the state and are also among the worst death rates in the country.
In 2017, there were 2,196 opioid-related overdose deaths in California (3), according to the California Department of Public Health. Of these overdoses, 70% were the result of prescription opioids, highlighting how the abuse of prescribed medications has impacted the state. On the whole, opioid-related overdose deaths increased in California from 4.83 per 100,000 in 2011 to 5.23 in 2017. This issue hasn’t improved and still requires additional problem-solving on the part of state and local agencies.
Current Initiatives to Combat and Reduce Overdose Deaths in California
In response to the current overdose epidemic, the California Health Care Foundation launched a statewide network in 2015 (4). It is comprised of 16 local coalitions in 23 counties with three main priorities:
- improve access to naloxone to reverse drug overdoses
- increase safe prescribing of opioids, and
- implement medication-assisted addiction treatment.
Eighteen months after the launch of the program, 90% of coalitions were able to adopt safer prescription guidelines to reduce the availability of these substances. Additionally, 75% increased access to naloxone, and 50% expanded their medication-assisted addiction treatment services.
The California Department of Public Health has also taken steps to reduce overdose deaths in the state by launching a Workgroup in 2014 made up of more than ten state agencies as a way to address this complex issue. (5) The Departments of Public Health, Justice, Consumer Affairs, Health Care Services, and others have collaborated to create a multi-phase plan to find a solution. Initiatives from this Workgroup include:
- increasing public awareness about the dangers of opioid medications,
- improving storage and disposal policies, and
- enhancing the state’s Prescription Drug Monitoring Program.
The Workgroup has identified three focus areas for collaborative efforts, which have included data sharing, awareness, and advancing policy solutions.
The California Department of Public Health has been proactive in applying for grants as a way to increase funding for its initiatives. California has received a Centers for Disease Control and Prevention grant. This is related to prescription drug overdose prevention in addition to several others.
Continued after infographic:
A Solution for the Individual: Seek Help Today
While these initiatives are certainly a step in the right direction, they are not a total solution for individuals struggling with a severe substance abuse addiction. Individuals seeking to resolve their addiction to opioids and other substances need to take their health into their own hands. Finding a sustainable solution to this crippling condition can make all the difference in one’s life. Selecting treatment centers that employ a holistic treatment model is a recommended option. They provide individuals with interventions that target the whole person.
To overcome deeply ingrained behaviors, we must address the root causes of why the condition started. Addiction is a complex, often multi-faceted condition. Therefore, it is critical to deal with all of the factors that precipitated this dependent behavior. A holistic treatment center an ideal choice for this kind of work in recovery.
If you are struggling with severe addiction and you want to address the problem before it gets out of control, contact Ocean Hills Recovery today. They will work to keep you focused on the path to recovery. We offer a solution-focused, holistic approach that we structure according to each person’s individual situation. Relapse doesn’t need to be viewed as a failure. Rather it can only become a success if you decide to take the next step and address the problem. Let the caring clinicians of Ocean Hills Recovery help you jumpstart the recovery process.
SOURCES:
(1) https://www.cdc.gov/drugoverdose/data/statedeaths.html
(2) http://www.uclaisap.org/ca-hubandspoke/docs/reports/Strategic%20Plan%20California%20Opioid%20STR%208-30-17.pdf
(3) https://www.cdph.ca.gov/Programs/CCDPHP/DCDIC/SACB/CDPH%20Document%20Library/Prescription%20Drug%20Overdose%20Program/Injury%20Data%20Brief%20Opioid%20Overdose%20Deaths%202011-2017_ADA.pdf
(4) https://www.phi.org/uploads/application/files/bt93oju0nrnbsmjhpdw692ljgu0d27ttdpzxmbclj7cxq99alz.pdf
(5) https://www.cdph.ca.gov/Programs/CCDPHP/DCDIC/SACB/CDPH%20Document%20Library/Prescription%20Drug%20Overdose%20Program/CAOpioidPreventionStrategies4.17.pdf